
Are you tired of struggling with constipation? In this episode, we dive deep into functional medicine to provide practical, holistic solutions for managing and preventing constipation. Discover how simple dietary changes, tailored supplements, and lifestyle adjustments can help you achieve regular bowel movements and improve your overall gut health.
Our experienced functional medicine experts will walk you through evidence-based strategies to address the root causes of constipation, such as imbalanced gut microbiota, inflammation, and dietary triggers. Don't let constipation hold you back any longer – watch this video and take the first step towards a healthier, happier digestive system today!
In this episode, we cover:
00:59 – Laxative “Tiktok Trend” for Weight Loss
05:37 – Conventional Approach to Constipation
11:07 – Wet Wipes Vs. Proper Cleaning
18:20 – Inflammatory Foods and Fibrous Foods
23:53 – Low Thyroid on Motility
33:31 – The Functional Medicine Approach
Dr. Justin Marchegiani: Hey guys, Dr. Justin Marchegiani here with Evan Brand today. We're going to be chatting about the root cause of constipation from a functional medicine perspective. We're going to give you our clinical pearls of Wisdom based on our combined total, maybe 30 years of clinical practice. Really excited to do today's podcast. Evan, how are we doing today, man?
Evan Brand: Hey, man. Doing well. And we were chatting pre-show when you look at the major complaints people bring to us, a lot of it is fatigue, weight, mood, skin, gut. And then you break down those gut symptoms, I would say the vast majority of people are dealing with constipation more so than diarrhea. You'll have people that have diarrhea every so often. It's kind of this weird, like, is it a gut bug cycle? Is there a parasite? Is it a full moon? You'll hear stuff like that. But constipation seems to be the majority. So hopefully, we can just showcase some of the clinical pearls you and I have learned and how we can fix this because I personally don't think it's that complicated.
Oh, by the way, did you know there's actually like a Miralax shortage in the US right now? And apparently, people in their 20s, 30s, the age groups that typically didn't use laxatives are now doing it. So if you type in like Miralax shortage, there was an article I just saw about it, and it says here, “Americans face laxative shortage due to high demand.” And then also a TikTok trend. So they're saying here, oh, here we go. So this maybe is why. It says here, “A wave of American teens are using laxatives as budget Ozempic as part of a TikTok trend.” So I guess they're trying to lose weight by just pooping all the time?
Dr. Justin Marchegiani: Interesting. And then with Ozempic, that's the blood sugar peptide medication, correct? And so does that have a side effect of constipation? Is that why they're using it?
Evan Brand: I'm not sure. It's saying here, (the counteractive side effect). I'm trying to see why someone would use that. Okay, I guess they're just doing it for weight loss. They're just hoping that they're gonna just poop more and lose weight. Yeah.
Dr. Justin Marchegiani: Yeah. I mean, that's just terrible. Because if you do that, you're gonna lose lots of electrolytes, lots of minerals, and you're not fixing anything. And it's not about you pooping stuff out; it's about your body metabolically partitioning fuel, right? Because its fuel comes into your body, right? Calories, nutrients, and there's like an air traffic controller that says, “Hey, go here to the mitochondria, get burnt up, go to the muscles, get burnt up, hey, go to the fat cells, and get stored.”
And just because you're taking what's left over in the stool and you're pushing it out, if you're trying to decrease calories to that, then you're going to have malabsorption. So you're going to have fats, vitamin deficiency, B vitamin deficiency, mineral efficiency that's going to impact your heart, your mitochondria. And so you really–it's really about getting your metabolism healthy enough so you can start telling your body, using that air traffic controller, to say, “Hey, calories, nutrients, go get burnt, go get burnt up, and do less of the storage thing.” Yeah. And that's important, so you really fix that.
Evan Brand: One other part of the article and then we can get geeky here. So it's saying here that, you know, a surprising number of younger adults are also using fiber supplements. So we need to talk about the whole fiber myth. I really don't do or push fiber at all, but here's what they're saying now: that a lot of these manufacturers, the manufacturer of Benefiber, is now making a gummy version of their product now to appeal to young adults. And that apparently 18 to 42-year-olds are hopping on fiber supplements more than ever.
Dr. Justin Marchegiani: Interesting. Well, let's dive in. I mean, first off, if we look at conventional medicine's approach, you already kind of talked about it with Miralax. Miralax is an osmotic; it's basically an anti-freeze derivative. If you look at it, it's like a polyethylene glycol; it's basically an anti-freeze derivative. So not the most healthy thing. It's an osmotic, so it's going to pull water out with it and so that's going to increase the water in the bowels and then help move the stool out faster. But that's not fixing a lot of things.
Also, in the colon, you're going to reabsorb a lot of your electrolytes there, and so you're going to create lots of potential dehydration and electrolyte issues which can impact your sodium-potassium pump, can impact your muscles, your muscle contraction, again, your heart because your heart needs all these good electrolytes: magnesium, potassium, healthy sodium chloride, minerals for the heart to function, for your cells to communicate. So really important stuff.
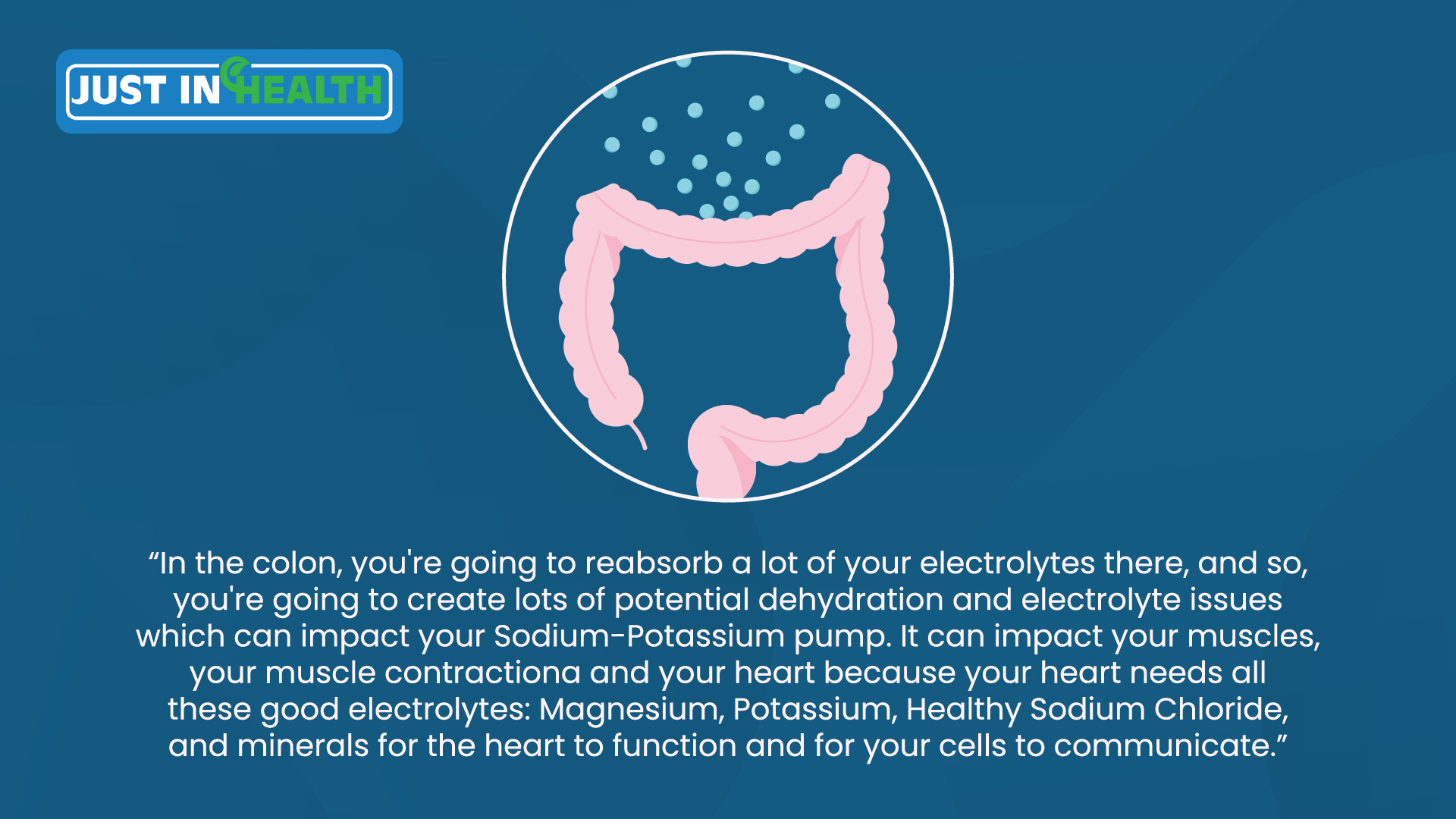
Evan Brand: Yeah it's amazing that you're able to conceal a chemical like that by putting such a strong brand. Like if you say Miralax, you know it's almost like Kleenex for tissues, right? Like, everyone just associates that as this magical remedy to make you poop. But yeah, you break down the ingredient, you're exactly right, that's what it is. (Yeah not good.)
When we see people, we like to do a workup on them first. We like to get some data. Our preferences have labs. Let's look at those and then figure out why the motility issues are occurring rather than we could easily throw you on some magnesium hydroxide, which is maybe the competitor to Miralax, which is far superior because it's magnesium, it's just a type of magnesium that will draw water to the bowel. So magnesium hydroxide, we could easily throw that at you and say, “Hey, try this and it'll probably help.” But there's likely something that's happening underneath the hood that's really going to drive the constipation.
So we'll look at organic acids testing, we could break that down and then also stool testing, we can find a lot. And what we find is that certain bugs are going to cause more diarrhea issues and certain bugs are going to cause more constipation issues dependent upon the toxins, the gases they're releasing. Once we fix the gut dysbiosis, 99 out of 100 times, motility is no longer an issue.
Dr. Justin Marchegiani: 100%. Now I like to just compare people's experience. You go to a conventional medical doctor, what happens? You say, “I've got constipation.” First off, right? They're going to look at you and they're going to say, “Okay, constipation. Miralax.” They'll have their list of laxatives; they're going to prescribe probably from least invasive to more invasive, right? They're going to start with Miralax or something over the counter, maybe they add in some kind of a psyllium fiber supplement, something very simple like that, that's most of the time.
Okay, now they may ask a bunch of questions to basically rule out any IBD, irritable bowel issues. Is there blood in the stool? Is there pain? Is there inflammation? More than likely, they're going to just put you in the IBS-C camp, which is irritable bowel syndrome C, and that's just a diagnosis of exclusion. They rule out all serious stuff, ulcers, Crohn's, any irritable bowel disease, any significant inflammation, blood in the stool, cancers; they're going to rule out all the big stuff and then you're kind of left with the IBS or IBC camp. IBS is going to be, or I should say IBD is going to be irritable bowel, that means they've ruled out everything else with diarrhea, or IBC, which is irritable bowel with constipation.
And so it's kind of a BS diagnosis because they know something's there and they're just spot treating the symptoms. “Oh, you're nauseous? Nausea? Oh, there's a little bit of tummy upset, indigestion, acid blocker. Oh, you have a little diarrhea? Right, have some Pepto-Bismol. Are you having a little bit of this? Have some Miralax.” And they're just spot treating the symptoms with the drug. It's pretty cookbook, simple, right? There's no root cause; there's no explanation; there's no thought process of how do we get here and how can we reverse it?
Now the problem with a lot of these situations is a lot of times these medications are going to further create more bacterial imbalances which are driving the issue, and they're going to further create more nutrient deficiencies, like I mentioned before. It's going to further exacerbate sodium-potassium-magnesium deficiencies, which then can create more neurological issues, more heart issues, more adrenal issues, and then you'll go back next year or two years with more symptoms, and then you'll get more Band-Aid medication.
So you can see how it's kind of the gateway to more symptoms which then puts more medications, which then puts more symptoms. So it's this vicious cycle when you go the conventional route. If you're looking for a long-term solution with their Band-Aid option, you're going to just get stacked a lot of other supplements or a lot of other medications over time that create more problems.
Now, on the functional medicine side, there's the root cause perspective, which we're going to be talking about today, and there's palliative support as well. Like, palliative support could be oxygenated or magnesium oxide or magnesium citrate to tolerance. It could be trifola; it could be artichoke; it could be ginger; it could be some bitters; it could be … magnesium. You could do some vitamin C as well, right? There's a lot of nutrients that you can do that would cause a little osmotic effect; there's some herbs that you can do that are a little more abrasive like senna or cascara sagrada. There are some gentle fruits like artichoke or like trifola, which is a fruit as well; they work really well for gently nudging the bowel in the right section. You could even add in some prunes or some prune powder. These are some natural, kind of palliative options.
Now, I always say palliative because it's not fixing the root cause, but if you combine it with a comprehensive program, it can be part of something that gives the patient relief faster, and also, when we do gut killing to knock down microbes, that's super helpful because we do not want to be reabsorbing microbes because our bowel is too slow. So it can be a really important part that allows the root cause to come in faster with less pain and symptoms.
Evan Brand: Yeah. So what is constipation? I mean, me, I would just classify it as not pooping every day. Our goal for people is you gotta poop at least once a day, preferably twice a day, maybe even three times. Now, you start getting five, six, seven a day, that's too many. That's definitely more IBS territory. But if you're not going every day, I would just classify that as constipation. I don't know what the conventional medical world calls it, but to me, it's not going every day because we know that as you mentioned when we're killing bugs, we've got issues there where we've got to get that stuff flushed out. If we're taking binders because we have metals, pesticides, chemicals, mold toxins, we've got to be flushing that stuff out. So to me, at least once a day is the goal.
Dr. Justin Marchegiani: Yeah. I would say 12-inch stool every day. And so you can test it with a Transit time test. You can do some beets which will make your stool red, and you want to be 18 to 24 hours, you want that redness out of your stool. So time it, look for your stools to go red. “Oh, it's red in 12 or 16 hours.” Twenty-four hours, it should be fully out, no more red in the stool. You can do it with charcoal and look for black stool; right? Charcoal can be a little bit more slow in the motility so I like the B test, that's nice. So, we want to see the transit time 12 inches in 24 hours. I want to see the red out within 24.
And then also, I'll look at evacuation. Do you have to really strain to evacuate? Are you that Bristol stool chart one or two where it's like pellety, like kind of rabbit pellets? So, I'll look at the pellet consistency. Is it consistently pellety? Do you have to really bear down to move it? Is it a difficult evacuation? And are you just not passing enough stool in that 24-hour period?
Evan Brand: Yeah, and then obviously you could have hemorrhoids if you're pushing too hard. So now you've got to deal with that. Now you're back to Preparation H, and now you're back at the doctor asking for magical creams for your butt. So, you know, this is, as you see and as you elucidated, it is a slippery slope of one thing to the other. These other Band-Aids, and then, you know, people with wet wipes too. I've seen that as a common thing. Is that you really shouldn't need wet wipes.
I mean, the goal is, I call it a ghost poop. You wipe your butt, and there's nothing there. Maybe if you're using a bidet it doesn't count, but like really it shouldn't be this huge process to get yourself clean. That's another problem that comes with these motility problems is people just have bad consistency of their stool too. It should really be pretty much banana shape, size consistency, pretty easy to get out. It shouldn't be this huge ordeal where you've got to take your phone in there and you're on TikTok for 20 minutes. Like if you have time to be on your phone while you're pooping, then it possibly is taking too long.
Dr. Justin Marchegiani: Yeah, I mean, I'm a big fan. You know, you should just be able to move that bowel, and there shouldn't be a ton of wiping. The ton of wiping is usually because of the fat in the stool. So I'm a big fan of using bidets. It's like taking a shower every single time you have a poop. It's just more sanitary, more clean, and it's just easier, especially if you are having bowel motility and you are going four or five times a day. Sometimes the wiping can be a little bit irritating if you're on the fence of having hemorrhoids. So, if you have hemorrhoids or you're close to it in that area, using a bidet is much more gentle. And then you can do it right after you have your BM, you have your BM, you flip the switch 5-10 seconds, and then it's clean.
Because I see it with my kids, right? I'm not sure you have it happen. They go in the bathroom, they have their number two, whatever. They sit for 10 minutes, and they're like, “I need help wiping,” and then everything's all dry. And I'm just like, “Oh my gosh.” And then I have to do wet wipes because everything's just like, you know, you can't. So it's just a disaster, right? So obviously bidet, wonderful for that, less irritation on that rectum, anus area. So much better from an inflammatory standpoint.
Now, you were talking about here, you're talking about the wiping, right? So if we're seeing that, it means there's not fat being digested properly. So that's where we're going to be plugging in more hydrochloric acid, more enzymes, especially enzymes that are high in lipase because lipase helps break down fat. And we may want to add in bile support too. So, are you having that upper right quadrant pain at all? Is there any inflammation up there, right? Do your stools float? Do they look gray or blonde colored? So that's where we want to plug in bile.
Now, if you don't have enough bile, guess what? Bile has a mild acidic aspect to it. It's why it's bile acid, and it creates an antimicrobial environment. And you need hydrochloric acid to also create an antimicrobial environment. Hydrochloric acid will knock down bugs. That's why any natural cleaner recipe is usually citrus-based or vinegar-based, which is acidic, right? Citric acid or acetic acid. So it helps knock down bugs. So it activates your enzymes. Enzymes are all acidic-based, so low pH activates your enzymes, also knocks down the microbes. So it starts the digestion going. It keeps your stomach a little bit cleaner. It keeps your small intestine a little bit cleaner from a microbial standpoint.
And then that acidity triggers the closing of that esophagus so acid does not rise up. And that's part of the reason why you see low acid environments can actually trigger acid reflux because it helps one close that esophageal sphincter, and it prevents the fermentation and rancidification of acids after the fact from those foods rotting in your stomach.
Evan Brand: Yeah, so if you had, let's say, burping, bloating, some sort of gastritis, that's going to be your term, happened to my father-in-law a few weeks ago. So, my wife's mom, she sends us a message. She's like, “Hey, your dad has this and this and that.” And, you know, I suggest back, okay, tell her this, tell her that. And then she's like, “Well, no, we're going to go get him checked out.” I'm like, he doesn't need to be checked out. This is going to be a total waste of time. So she doesn't listen. She goes, she gets him a colonoscopy. Obviously, that's anesthesia, not good on the brain. Then he gets an endoscopy. Obviously, not good because you can get a hospital-acquired infection. So pseudomonas and C. diff, there's other bacteria you can get just from a simple procedure like an endoscopy.
And guess what they come back with? Colonoscopy is perfect, no issues, but the esophagus is inflamed. And so they say gastritis and possibly getting into Barrett's esophagus, which as you and I know, this is like a chronic issue where there's been an issue with the sphincter, there's been some acid backwashing into the esophagus and has created damage. And so the only recommendation, acid blocker. I'm like, don't do it. Can't do it.
So, you know, I tried to save them from that, but, you know, you would think our families are like the healthiest people ever, but they don't listen to us in most cases.
Dr. Justin Marchegiani: So it says in the Bible, you're never a prophet in your own town. So it does not matter how much you know or how well-informed you are. Once people see you as little Evan or little Justin, and then you grow up, they still see you as that person or that kid, right? And they don't have the same level of respect right?
Evan Brand: Yeah, the long story short, though, was there's probably been this chronic issue in someone's life listening or watching in, and maybe you had that gastritis. So you do take that proton pump inhibitor. Now you've lowered the stomach acid. Now you see the issues like you're describing with the fat malabsorption or the fat digestion issues. And the cool thing is we can quantify this. So when we run your stool test, which if you're listening and you're going to work with us, we're going to want to run this stool test on you. It's far more advanced than what even your GI doctor at a hospital that's prestigious is going to look at.
And we can actually measure steatocrit. And this is your fecal fat in the stool. So we can quantify it. So if you say, “Hey, look, I'm leaving a mark in the toilet,” or “It's really messy,” or “It's floating,” well, we can look and go, “Oh yeah, your steatocrit is 32%. That's a problem. We've got to fix a problem.” When you get numbers like that, it really helps us to guide into the correct place. And then let's talk about the gut bug piece too, because pretty much 99 out of 100 people with some level of digestive issues, we're going to see something. It's going to be bacteria, yeast, fungus, parasites, worms, etc.
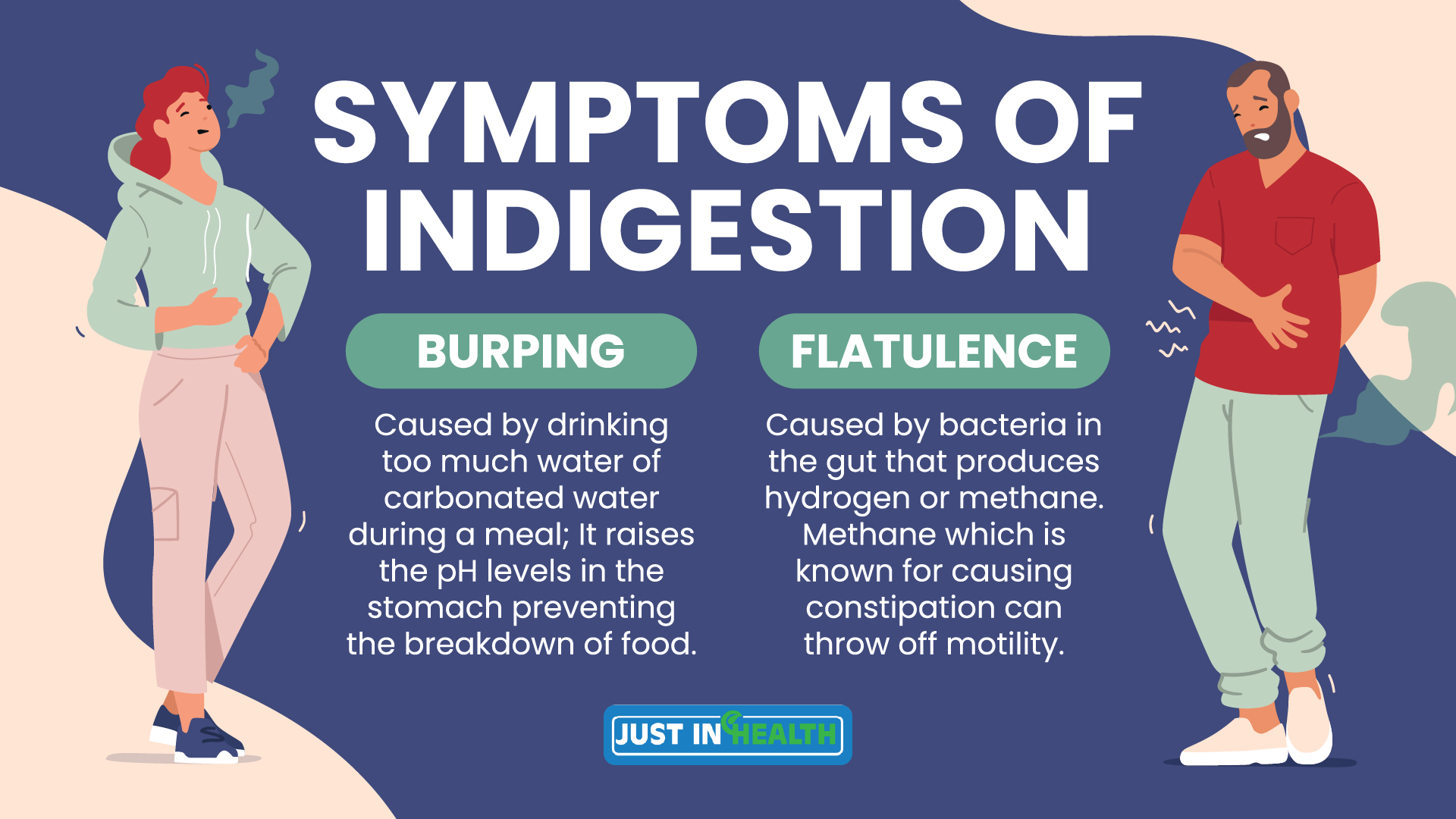
Dr. Justin Marchegiani: I want to just back up just one sec. So the first piece is, are you breaking down your food adequately? We talked about fat digestion, carbohydrate digestion, protein digestion. Are we breaking those foods down? We know we're having poor breakdown if we're excessively burping. Things aren't being broken down unless you're taking excessive water or carbonated water. That could be doing it too. And water will dilute your enzymes and your acids because water's a pH of seven. Your stomach should be a pH of two-ish. So that's going to raise the pH.
So burping means indigestion in the stomach. Got to look at enzymes, acids, bile salts. That's one. Two is, if you're having lots of flatulence downstream, now you're having more farting, flatulence. Now we know we're not breaking things down well downstream. And that's where the bacteria has a field day eating a lot of these microbes, and then they poop their own gases, whether it's hydrogen or methane. If it stinks, probably methane. Methane gases are notorious for causing constipation. They can throw off that whole migrating motor complex, which again, the vagus nerve and your healthy nervous system function plays an important role.
That's why if you're beating your adrenals up and you have adrenal issues and you have female hormone or male issues, the hormones have to play a role in healing because they help with the vagus nerve and the parasympathetic response, which then helps that migrating motor complex. That's why meditation or doing any of these DNRS or Gupta programs that help get the brain stem calm down can help.
Now, we skip one thing, the most important thing is obviously the food. If we're eating inflammatory food like gluten, like processed flowers, grains, junky omega-6 fatty acids, even too much carbohydrate, that can throw off one, it can inflame the gut, and it can also throw off the microbials. Go ahead.
Evan Brand: Yeah, what do you have to say about fiber? I mean, because I really don't push fiber at all. I really don't eat that much fiber. My motility is good. I have no issues, so I'm really not in the camp where I'm pushing a psyllium husk on someone. It is true that there's a little bit of pectin in some of the binders that we use, so maybe the pectin is helping with people as well. But beyond that, I'm not really pushing fiber. I'm not telling people you have to eat X servings of vegetables to increase your bowels. It's just really not necessary to me. It's not a necessary step. Now, if people like it, maybe go for it, but I don't find it as part of the protocol.
Dr. Justin Marchegiani: Well, I think it's one of those things where people get a benefit. It's not because they're eating it per se, but because they're not eating something else. So if someone is eating lots of processed grains or lots of processed sugar, and I'm like, “Hey, let's just sub those processed foods for healthier vegetables or some lower sugar fruit,” well, that's automatically better because the food's less inflammatory. There are some nice fibers which can't help, but they're also not feeding a lot of these bad microbes with the processed sugars too.
So it's kind of like, well, you're pulling this out, so you're getting a benefit because this isn't there, but you're also adding this, which does have more potassium and magnesium. So I think having vegetables, especially if they're having motility issues, as long as it's cooked and potentially lower FODMAP can't hurt. But I will add in specific fibers, but I'll do it more from the prebiotic phase of care, and we'll talk about that, which acts like fertilizer to help grow a lot of that good, healthy commensal normal bacteria.
So when we do gut killing programs, we'll knock down a lot of the dysbiotic stuff. We'll target the Citrobacter to the Klebsiella, the Pseudomonas, but sometimes that commensal bacteriality and Firmicutes, phyla bacteria get knocked down a little bit. And so we want to really work on building that up. So then the fibers that we give are going to help create more butyrate, and that butyrate kind of feeds the healthy bacteria, makes it harder for the bad bacteria to grow.
Evan Brand: Yeah, well said. Just to say it another way so people get it. What's happening is when we're coming in, we're not prescribing antibiotics, just to be clear. That could be maybe the conventional route if you're with the GI doctor. Maybe you get lucky, and they run a test, and you show up with a high enough level of pathogenic bacteria where they're going to suggest amoxicillin or rifaximin or some other sort of “conventional SIBO treatment”, okay? I'm using quotations here because I find the rifaximin and all these conventional drugs, they're just really not that good, and a lot of people relapse.
And so we're going to come in with the herbal medicines instead, and we're combining those. So we'll put together particular blends, and we've used these literally thousands of times. So there could be a case where you have a primary bacterial issue, but there's also some yeast and/or Candida or fungal issues. So now we're thinking, okay, we've got multiple bad guys here. We've got bacteria, and then we also have a yeast, fungal component. We're going to tailor those herbs specifically to that. Or we could see on this side, okay, it's a bacterial and parasitic issue. So now we're going to use more herbs for parasites and bacteria, and maybe there wasn't a fungal problem at all.
And while you're doing that, you will see some of the good guys die in the battle, die in the crossfire, if you will. And so, he mentioned the word commensal. So, commensal, your good guys, you'll see those. They can look lower on a retest, indicating, ‘Hey, some of your lactobacillus, your bifido, they've been knocked down,' and that's important to rebuild because those help you make B vitamins for energy. So, if we're tying in your constipation issues to your chronic fatigue or your anxiety or your depression or your skin issues, you gotta make sure you understand all these symptoms are linked. It's rarely just constipation. It's likely other things happening.
So, he's saying now we're going to throw in maybe some prebiotics or even some living probiotics at the time of killing or even after killing to make sure the good guys are put back in. I always use, like, the nightclub analogy. You know, you've got all these guys tearing up the club, and so you knock them out. But I use that for the mold analogy. What I say is like the back door is left open if there's still mold there, and the bugs and the scrubs move back into the club. But, in your case, what you're describing would be we're kicking these guys out, but then we're going to go ahead and put some good guys in the club so there's no more trouble.”
Dr. Justin Marchegiani: Hey, by the way, I got a dad joke.
Evan Brand: Tell me.
Dr. Justin Marchegiani: It's a functional medicine dad joke. (Okay) “Where is the main place dysbiotic bacteria party?”
Evan Brand: I don't have a clue. Go ahead.
Dr. Justin Marchegiani: “Club siella.”
That's a good one, dude. I just thought of that, like, in doctoral school, I thought of it one day. If my kids were there, they'd be like, ‘Oh, Dad!'
Evan Brand: That's hilarious.
Dr. Justin Marchegiani: That's a good one, right?' (Yeah) In this case, you guys didn't know it's klebsiella. It's about dysbiotic bacteria. The big ones that we see are klebsiella, pseudomonas, citrobacter, morganella, prevotella. These are some big ones. Streptococcus, staph we'll see them, you know, way overgrown. And again, these guys are gonna produce toxins like lipopolysaccharides or endotoxin that will disrupt motility. They will also take a lot of your good fermented nutrients from the healthy bacteria and eat it up.
And, of course, they will produce enzymes that make it harder to detoxify hormones. So, it'll produce beta-glucuronidase, which will take a lot of your hormones that you're trying to detoxify and package up and conjugate and it will deconjugate it, take the handcuffs apart and let them go back in. So, girls listening, you'll get estrogen dominance, you may get more acne and skin issues and hormonal issues. Guys, you can get the same kind of things going on there. And so, really important to get dysbiotic bacteria addressed.
Now, I didn't touch upon this yet, we missed it yet, but I want to make sure I hit it in here: low thyroid can play a major, major role with motility. So, thyroid hormone does play a role with that, stimulating that migrating motor complex. So, if we have a thyroid issue, when we have low T3, low T4, elevated TSH, maybe we're not converting. Most thyroid issues are Hashimoto's. So, guess what? That's immune-based, right? That means your immune system is attacking the thyroid, so you can lose function of those follicles from producing hormone. And so, most thyroid autoimmune conditions, guess what? They start in the gut.
So, you can see a gut issue can actually increase your chance of an autoimmune problem due to gut permeability, due to zonulin, due to this whole leaky gut, gastrointestinal permeability thing. That thing can feed back, it can tag a lot of the thyroid tissues because gluten and casein and a lot of these foods look similar. And also, bacteria like H. pylori and Blasto and Yersinia can look similar that triggers the immune response to start going after these proteins here, these surface proteins. And they can attack the tissue, which can lower thyroid hormone, which can then decrease thyroid output, and that can decrease motility.
So, you can see when you go into your MD for a five-minute appointment about constipation and they're just like, ‘Here's some Miralax,' you can see how totally incomplete this is in regards to getting to the root cause or having a long-term plan of attack to fix the underlying issues. And it's not one issue; it's five or six or seven or eight issues. And this is why functional medicine does not perform well in clinical trials because when you do a study, it's double-blind, there has to be one variable that you control. We're controlling 10, 15 variables. I don't have time to just say, ‘Hey, take some magnesium,' or just pull this one food out.
We're pulling all kinds of diet changes. We're going low FODMAP, we're cooking foods, we're getting digestive support lined up, we're getting probiotics lined up, we're getting gut killers lined up to knock down this body bacteria. So, there's so many variables. And this is why people that go and look at scientific research a lot of times, there's only one isolated variable. So, it's the slow boat to really creating change because when we're creating clinical change, there's so many variables that we're working with. And we can't just isolate one because it'll take too long.
Evan Brand: Yeah. Well said. I actually had a girl that came into the clinic last week. She was 13 years old. She's already dealing with weight issues, and her TPO antibodies are off the chart. So, 13 years old with Hashimoto's. We did find klebsiella on the stool tests. She had other bacterial issues as well. So, this is not just a problem affecting women 40 and up. I mean, we're seeing this in female teenagers all the time. Unfortunately, I've even seen it in girls under the age of 10 that are already dealing with motility and thyroid and autoimmune problems.
So, this is becoming a much, much bigger problem for the youth. If you look at the statistics, even from the CDC, which, you know, whatever you feel about them, but they have statistics on childhood illness and chronic illness in children, and it's becoming massive. I mean, it is literally a hockey stick where now the numbers they're looking worse, but at some point in the near future, it'll be half of all children will have some level of chronic illness. And so, this is really a train that's running over the Grand Canyon with no bridge to cross.
So, we really have to do our job here and implement these nutritional strategies, get the kids pooping, get the adults pooping, get the motility problems figured out, get the acid and enzymes restored, get the infections gone, and, you know, you and I've seen things get worse even in just the last five years with people. People are just too stressed, they're too burned out. You mentioned the adrenal component, obviously, there's the adrenal thyroid connection as well. (Yup exactly.) So now your thyroid could potentially be downregulated as a protective response because you've just been burning the candle at both ends for so long.
So, this is where not only are we working on the gut, but now we're using nutrients to stabilize and support the adrenals, to stabilize and support the thyroid. And this is really what makes a full complete protocol to where people can reverse these problems and live a healthy life. I know it's very easy to be pessimistic in the modern world, and you look around at society, and, you know, me personally, I look at where things are headed, and I don't like it. I don't like seeing the amount of illness, I don't like seeing the amount of people suffering. I mean, it seems like everywhere I go, somebody has a cast on, like, they broke the wrist, or you hear about someone's mother falling and breaking their hip.
It's like we've become so weak and so nutrient-depleted, and you and I've done thousands of organic acid and nutrient profiles, and even people that are eating carnivore, animal-based, 100% organic, autoimmune paleo, paleo, whatever, like any flavor of healthy nutrition, those people still have nutrient deficiencies and issues. So, don't think that you can eat your way out of this. I really, really want to hit that because, you know, on social media now, there's so many people talking nutrition, nutrition, nutrition, like it's so popular now where someone's standing in the grocery aisle, and they're like, ‘Don't eat this, eat this,' or, ‘This is bad because this,' and look at this ingredient. It's like you can hyper-focus on all the freaking nutrition stuff you want and still not fix these issues right here.
Dr. Justin Marchegiani: Yep. And even with some of the herbal supports that we use to go knock down microbes, by the way, great job on that. I totally agree. And people are getting sicker. I see it every single day. I have young kids, so I see what other kids eat, and it's really atrocious. Kids don't eat protein anymore. They have massive blood sugar issues. They literally live on a blood sugar roller coaster. Twenty percent of fifth-grade boys are on some kind of SSRI or Adderall or Ritalin or some kind of upper or downer for mental issues. So, it's just, it's sad, right? And these drugs have massive impacts on frontal cortex development, and it's just sad that you have lots of kids, young kids, living their entire life on some of these medications.
We don't really know what that's going to do to a brain when you're on that your entire life. There's no long-term studies on this stuff. So, it's really concerning. But just getting back to the constipation thing, I never recommend clearing herbs, antimicrobials until we've gotten the digestion, the absorption, and the motility better because when you start killing a lot of bugs and you don't have the motility dialed in yet, you're going to reabsorb so many toxins. You're going to be brain fog, fatigued, tired. It's going to be terrible. So, anyone listening, please, it's very important. You need to work with a functional medicine provider before you just throw a bunch of things in there because you can make yourself feel very worse, especially if you have a lot of junk dysbiosis in the gut. You can really make yourself feel worse energy-wise, constipation-wise, cognitive-wise if you just start throwing a whole bunch of herbs at your gut.
Evan Brand: Yeah, well, it's become more common now, this idea of like a parasite cleanse. It's become kind of trendy in the sense that people just go and they buy these kind of pre-boxed kits, and it's four, five, six different things, and they take it, and then they come to us later and they're like, ‘Hey, that flared up my skin. Now I can't sleep. I have insomnia now. Now I have all this anxiety. What do I do?' And it's like, well, did you do any labs? Do you even have a clue what you're going after? Do you even know you have parasites? No, but, you know, they said during a full moon this and that, and that sounded like me.
And so, there's people out there that are kind of shooing away or poo-pooing this idea of getting clinical data, and I think it's a mistake. And, you know, my story, and I've told it many times, just about Micah and how I had various infections, and if I wouldn't have run labs, I wouldn't have had a clue. And I was taking oregano and other things to try to spot treat, but I didn't have the full picture, and therefore, I didn't have the full plan to get better.
Dr. Justin Marchegiani: Exactly. And that's why it's really easy to be like, ‘Oh, I'm gonna just take some magnesium oxide or some trifola to help my motility.' But are you improving your digestion? Are you improving your absorption? Is your gastric tissue or intestinal tissue inflamed? Do you have elevated calprotectin or eosinophilic protein? Do you have immune mucosal barrier weakness, right? Are you having reflux? All these things. Are your adrenals beaten up? Because we know we can just go and beat up the gut, knock down microbes, but if that HPA axis, that adrenal axis, that parasympathetic nervous system response is depleted, it's going to be hard.
You're going to have a lot of relapse because your nervous system is so sensitive, increase of food allergens and allergens in the environment. So, you really gotta look at things holistically. So, you want to look at your hormones, you want to look at digestion, and your ability to break foods down, you want to look at your gut lining integrity. Then we may look at herbs and nutrients to help with the gut lining. Any of my patients listening, I put a lot of ginger tea into the protocol with Manuka honey because that's very helpful for gut lining integrity. It's a mild antibacterial, and ginger is a wonderful prokinetic.
So, when I look at studies, I'm like, ‘Oh, ginger is showing to be better than other pharmaceutical prokinetics to help with motility. Interesting. I'm going to make that part of my protocol.' Right? So, I'll take research on different nutrients or herbs or microbes, and I'll be like, ‘Oh, I'm going to plug that into this comprehensive program.' So, that's kind of how I look at research. I take a small piece, and I plug it in. But there's not going to be research that gives you the program. You take one piece of that, and then you can plug it into your program.
Evan Brand: Yeah, yeah. Well said. If people haven't gotten data, or if your data is outdated, I had a woman yesterday, so, you know, we do these free intro calls with people, we talk to them about their issues, see if we can help. I had a woman yesterday, and she's like, ‘Yeah, I ran a stool test in 2014. Can we use that?' So for folks listening, we're in 2023 – almost 2024. You're talking almost a decade ago she had a stool test and she wanted to use that.
So, the answer would be no. I mean, if there's something crazy there that you want to show me, maybe, sure, I'll take a look, but in general, even in as short as a six-month time period, we can see a totally different picture when it comes to microbes in the gut, infections, gut inflammation, etc. So, I think it's really wise if you haven't already, get some recent labs run. Let us help you walk through those, and we'll make a plan to get your life back. This is going to change everything. I know you and I focus a lot on the symptoms, but really, it's important to highlight what is this doing in your real life?
Well, if you have better motility, you probably have better energy. If you have better energy, you're probably more successful and productive in your business, your entrepreneurship, your job. You're probably a better spouse to be around because you're less irritable, you're less grumpy. Maybe your sex drive is better because you feel better, you feel sexier because you don't have giant hemorrhoids coming out of your butt. So, all these things improve your personal life, your relationships, your financial, etc.
So, don't get so obsessed with the health piece that you forget what this is all about. This is really all about being a good functioning human where you could go take a bike ride without pain, where you could go swimming and not have any bowel issues, you could go to a theme park for the day with your kids, and you feel good enough to do that, and you're pain-free enough to walk three miles. So, this is what it's all about. If you really want to reach out, get help, it's easy to do. We work worldwide. It's incredible. It's so fun that you and I were ahead of the curve with telemedicine over a decade ago, and so now it's becoming more accepted, but there's literally no discount or no lack of help because it's virtual.
The labs we send to your door, you send those back, we get results, we go through it, we make a protocol. So, if you want to reach out, you can reach Dr. J, that's Dr. Justin Marchegiani, at justinhealth.com. So, justinhealth.com, or me, Evan Brand, evanbrand.com. Reach out to us, let us know what's going on, we can help facilitate labs if you need those, if you need updated ones or just have never had this, this is all new to you, organic acids, DNA stool, this is new stuff to you, we're happy to be the person to shine the light on your issues, why they're happening, and then we'll help you fix them.
Dr. Justin Marchegiani: Totally agree, really good points. evanbrand.com for Evan, justinhealth.com for me, schedule worldwide. I see lots of people. They recommend, because colon cancer is the number three cause of death for men, I think for most people, they get sick, number three-ish, it goes, I think it's like, I think it's like lung cancer, and then you have breast and prostate, go back and forth from men and women, and I think it's that colonic, number three.
Most people are just talking about early detection mechanisms, like colonoscopy, and then snipping off pre-cancerous polyps is kind of like preventative medicine. But I look at preventative medicine as doing things that actually reverse the reason why that thing grew, while you have growth in your colon to begin with, not just snipping it, because that's just early treatment versus preventative treatment, right? And so, I think there's other ways that we can look at things, using gut testing, using functional medicine principles and philosophy to actually get to the root cause, because we know if there's inflammation, if we know there's malabsorption, if we know the immune system is overactive, the chance that cancer cells and things that impact overall gut health in the long term are going to be present.
So, if we can use markers that are more sensitive, and we can use functional markers, and we can support digestion, absorption, get inflammation down, get absorption better, get gut permeability better, get gut and immune health better, because 80 percent of your immune system's in your gut, small intestine, stomach, etc., that's going to make a huge difference for disease prevention in the long run as well, not outside of just what someone may do with a colonoscopy and just snipping off some polyps, if you will, too.
Evan Brand: Yeah quick numbers then we'll end it here. So yeah, American Cancer Society says here: leading causes of death from cancer for males would be a lung and bronchus. They just call it bronchus cancer. And then second would be prostate and then right behind it is colon cancer.
Dr. Justin Marchegiani: Good. Facts are right. Good. Yep. So it's good to think about and again conventional medicine is- just get your colonoscopy start at 45 now. Okay you're sniffing a polyp, that is helpful but you're still not getting to the root cause of why that polyp is growing. And colonoscopies have their side effects. You're getting anesthesia which can wipe out lots of bacteria and can throw gut bacterial balance off. I've seen many people with massive side effects post-colonoscopy. I'm not saying you shouldn't do it. I'm just saying if you're low risk and you want to get an assessment start with a more non-invasive assessment first before you go into more invasive things. That's all I'm saying.
Evan Brand: Yeah, there are several studies, you can just Google it for yourself, anesthesia gut dysbiosis, top paper pulls up in a psychopharmacology article. They call it here, ‘General anesthesia bullies the gut,' (Yeah) and then they talk about this toxic relationship between dysbiosis and neurodegenerative conditions. So, we didn't hit on that today, we'll do a future show on that, but the next paper is ‘A toxic relationship with dysbiosis and cognitive dysfunction,' talking about how anesthesia has a major role in gut microbiotic composition, and it can massively change that, which then leads to cognitive dysfunction. So, let's do another gut-brain show soon.
Dr. Justin Marchegiani: So, my philosophy is if you're high risk for colon cancer, sure, go get a colonoscopy, do what your doctor says. But get to the root cause, address things from a root cause perspective. Don't just think, ‘I'm snipping off these pre-cancerous polyps, I'm good, right?' It's not that simple. You're not addressing any of the reason why these things are growing, right? So, go get some comprehensive functional medicine assessment, get to the root.
If you're lower risk, that's where I'd be leaning on more of these functional diagnostic kind of assessments that look at the function of your intestinal tract, some of the stool testing that we talk about, that's also non-invasive, doesn't have the anesthesia that can also throw off the gut bacteria more. Hope that makes sense. Again, you know, everyone's a little bit different, so go talk to your doctor about it, and again, we're just some talking heads online, we have a lot of experience, but if you want to dive in deeper from a doctor-patient relationship, feel free, links down below for Evan and myself, Dr. J, if you want to dive in deeper and really get to the root of what's happening here with your motility and gut health.
Evan Brand: All right, man, good job, take care.
Dr. Justin Marchegiani: Hey, Evan, great chatting with you, man. Take care, y'all, Bye.
References:
Schedule a FREE Consult:
http://www.justinhealth.com/free-consultation
Review us at:
http://www.beyondwellnessradio.com/itunes
justinhealth.com/itunes