

By Dr. Justin Marchegiani
In part 1 of this series, we talked about the adrenal and thyroid connection and how it can contribute to fatigue, weight gain, and mood issues. Adrenal fatigue and thyroid imbalances are some of the most common conditions I see my office. If you have two or more of the symptoms listed below, there's a good chance you have adrenal and thyroid issues!

My recommendation for anyone who has adrenal fatigue is to seriously curtail his or her exercise. The most common type of exercise is long, slow cardio, and it is shown to increase cortisol production by the adrenal glands. Therefore, it's important to engage in exercises that aren't as cortisol dependent (6, 7). The goal for any exercise should be to stimulate hormones that are going to change your body composition for the better. One of cortisol's main jobs is to liberate blood glucose. This is normally done through breaking down muscle into glucose. So if you continue to participate in long, slow aerobic exercise, over time you become fatter and flabbier. Not a good combination!
If you need help fixing your adrenal fatigue, click here!
Cortisol also has deleterious effects on your immune system, too, so if you find yourself getting sick frequently, you may want to think about changing the types of exercise you participate in (4,5,6).
Depending on how fatigued you are, walking and lighter exercise, like tai chi, may be all you can handle.
My overall exercise prescription has two criteria.
If you are in total adrenal fatigue, keep exercise duration to 30 minutes or less by using either resistance training or some type of interval- or burst-training workout that allows for high intensity for 20 to 30 seconds followed by a minute to two minutes of relaxation and rest. These types of exercise promote growth hormone and are not stimulating cortisol production as much as the conventional long, slow aerobic exercise.
I already mentioned above how important blood sugar stability is. I encounter many patients who think they're doing everything right, but when I look at their food diary, I can tell their blood sugar is in trouble.
One of the most important jobs of your endocrine system is to stabilize blood sugar.
Therefore, when you're skipping breakfast, not eating enough healthy fats and proteins, or going too long between meals, you're putting a tremendous amount of stress on your body. It's really hard for people to get this concept regarding blood-sugar stability, but it's one of the most insidious stressors I see in people with hormonal related issues. In other words if you do not fix your blood-sugar stability, it will be almost impossible to bring your hormones back into balance.
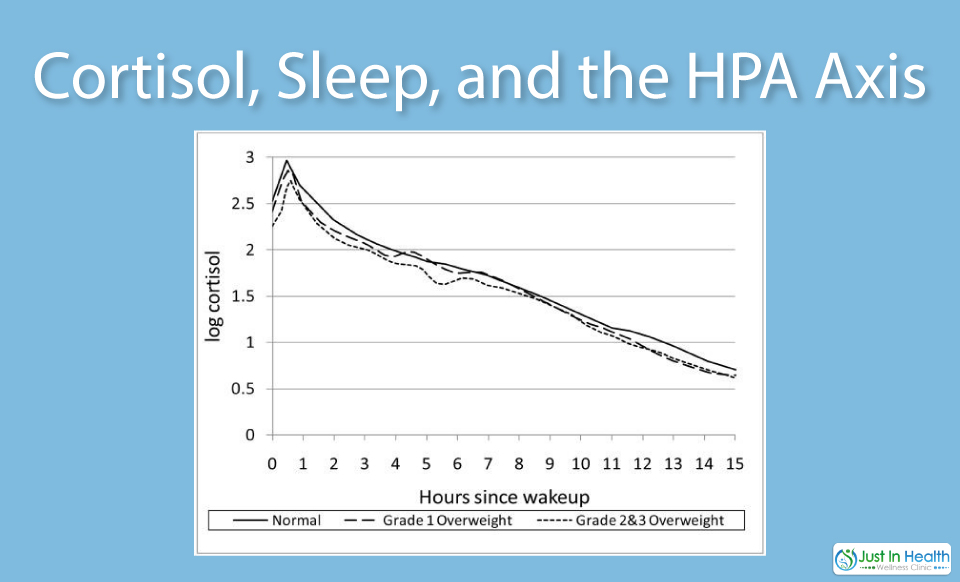
Sleep debt can impair cortisol balance as well. Getting five hours of sleep a night can cause cortisol to go out of balance and also put your body in a state of insulin resistance. What this means is it's very difficult for your body to bring glucose into the cell to burn it for fuel. Therefore, your blood sugar ebbs and flows more causing more stress on your adrenals to help stabilize that pleasure. Metabolic ward studies have been done on patients inflicting sleep debt and then running a glucose-tolerance test. The results tend to be a state of insulin resistance for the patients very similar to a diabetic. Therefore, stabilizing your blood sugar will help your cells to be more sensitive to insulin. The more sensitive to insulin you are, the less your body will store calories as fat. The more you're relying on fat for energy, the less your cortisol systems will be stressed (2).
Sleep loss could thus affect the resiliency of the stress response and may accelerate the development of metabolic and cognitive consequences of glucocorticoid excess.
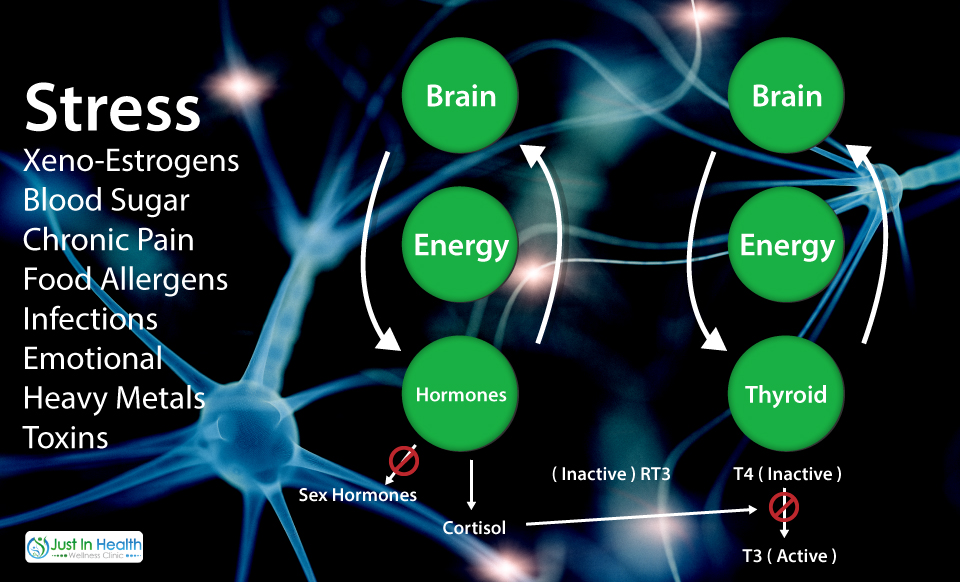
It's really important to know, over time your adrenal glands and thyroid gland don't just become fatigued from the stress you are putting on them but there is literally a state of dysregulation involving the communication from your brain to your thyroid and adrenals.
This is known as HPA (hypothalmus pituitary adrenal) axis dysregulation or HPT (hypothalmus pituitary thyroid) axis dysregulation. In other words imagine a broken thermostat. As the temperature in the house goes up, the AC doesn't kick on because the thermostat is broken. Just as the opposite is true when the temperature gets too low: the heat doesn't kick on because the thermostat is broken. This analogy rings true regarding your adrenals and thyroid as well (1).
Reducing cortisol levels and stabilizing HPA axis dysfunction can be a very effective approach to addressing sleep disturbances while also reducing the long-term risks associated with elevated cortisol levels.
The most important thing you can do is get your adrenals assessed so customized supplements and nutritional- and herbal-medicine protocols can be created specific to your adrenal pattern. The overall goal in treatment is to help lower inflammation, give your adrenals time to rest, and help the adrenals in the brain communicate better. Making the diet lifestyle changes and following a comprehensive program will help ensure that you feel better faster and don't slip back into old patterns that got you there in the first place.
To help get your adrenal glands back on track, click here!
1. The Role of Cortisol in Sleep,Tori Hudson, ND, and Bradley Bush, ND. “The hypothalamic-pituitary-adrenal (HPA) axis interacts with sleep in multiple ways. This article reviews the effects of the HPA axis on sleep and the converse.”
2. Sleep. 1997 Sleep loss results in an elevation of cortisol levels the next evening, PMID:9415946
3. Manna, I., Jana, K., Samanta, P. Intensive Swimming Exercise-Induced Oxidative Stress and Reproductive Dysfunction in Male Wistar Rats: Protective Role of Alpha-Tocopherol Succinate. Canadian Journal of Applied Physiology. April 2004. 29(2), 172-185.
4. Cakir-Atabek, H., Demir, S., Pinarbassili, R., Bunduz, N. Effects of Different Resistance Training Intensity on Indices of Oxidative Stress. Journal of Strength and Conditioning Research. September 2010. 24(9), 2491-2498.
5. Walsh, N., Gleeson, M., et al. Position Statement. Part One: Immune Function and Exercise. Exercise Immunology Review.
6. Shojaei, E., Farajoy, A., et al. Effect of Moderate Aerobic Cycling on Some Systemic Inflammatory Markers in Healthy Active Collegiate Men. International Journal of General Medicine. January 2011. 24(2), 79-84.
7. Steroids. 2011 Evaluation of a method to measure long term cortisol levels. Manenschijn L, Koper JW, Lamberts SW, van Rossum EF.